Five rapid-fire takeaways
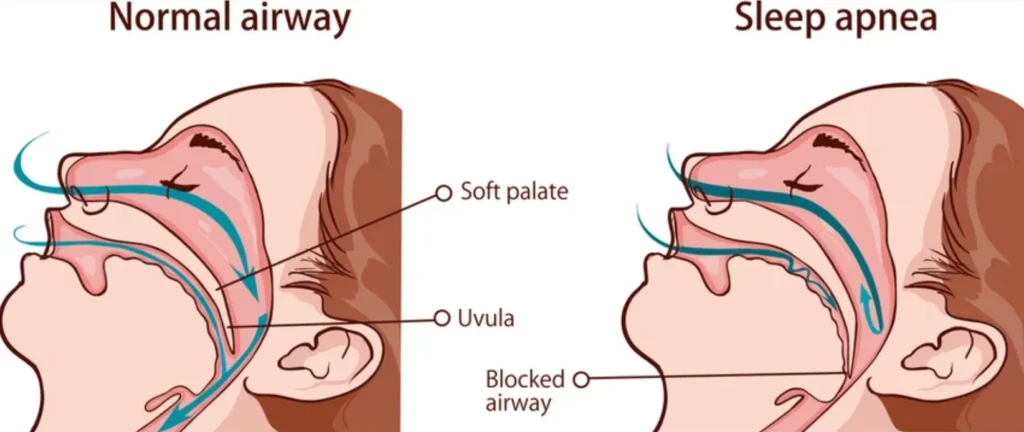
- Snoring is a sleep-quality problem first, and a “noise problem” second.
- Skip risky hacks. Start with low-drama changes you can measure.
- An anti snoring mouthpiece can help when the issue is airway narrowing during sleep.
- If you see red flags (gasping, pauses, severe sleepiness), screen for sleep apnea.
- Document what you try. It keeps you consistent and helps a clinician if you need one.
Overview: Why snoring is trending again (and why you should care)
Snoring keeps popping up in wellness feeds because people are tired. Travel fatigue is back, schedules are messy, and burnout doesn’t stop at bedtime. Add a partner who’s “joking” about moving to the couch, and suddenly sleep health feels urgent.
Recent sleep-gadget chatter has also pushed people toward quick fixes. Some headlines are nudging readers away from mouth taping and toward safer, more practical approaches. That’s a good shift. Your goal is better breathing and better sleep, not a viral experiment.
Snoring can be benign, but it can also overlap with obstructive sleep apnea (OSA). OSA is a medical condition that involves repeated airway blockage during sleep. If you suspect it, don’t treat snoring like a DIY-only project.
Timing: When to act now vs. when to get screened first
Act now (self-check + simple changes) if:
- Snoring is new after weight change, alcohol use, congestion, or a travel-heavy month.
- You feel “not great” in the morning, but not dangerously sleepy.
- Your partner reports snoring without clear breathing pauses.
Screen first (don’t delay) if any red flags show up:
- Choking, gasping, or witnessed pauses in breathing.
- High daytime sleepiness, dozing while driving, or morning headaches.
- High blood pressure or heart concerns alongside loud, persistent snoring.
If you want a reputable overview of warning signs, see Forget mouth taping — these 3 things will actually help you stop snoring in 2026. Use it as a screening checklist, not a self-diagnosis tool.
Supplies: What you need for a clean, low-risk snoring experiment
- Notes app or paper log: bedtime, wake time, alcohol, congestion, snoring rating (1–10).
- Phone audio recording (optional): confirm whether changes are real.
- Nasal support basics: saline rinse or strips if congestion is a pattern.
- Side-sleep support: a body pillow or backpack-style positional aid.
- Anti-snoring mouthpiece: if your pattern suggests mouth breathing or throat collapse.
Keep it simple. Too many variables turns your week into a guessing game.
Step-by-step (ICI): Identify → Choose → Implement
I — Identify your snoring pattern (3 nights)
For three nights, don’t change anything. Track:
- Sleep position (back vs. side)
- Alcohol within 4 hours of bed
- Nasal congestion or allergies
- How you feel in the morning (headache, dry mouth, grogginess)
- Partner report: “steady rumble” vs. “snort + silence + gasp”
This is your baseline. It also helps you avoid placebo decisions driven by frustration.
C — Choose your first lever (pick one)
Use the baseline to pick the most likely driver:
- Back-sleeping snoring: start with positional changes.
- Congestion-driven snoring: focus on nasal airflow and bedroom triggers.
- Dry mouth + loud snoring: consider an anti snoring mouthpiece and reduce alcohol late.
Yes, you can stack tactics later. Start with one so you can tell what works.
I — Implement for 14 nights and document choices
Week 1: Foundation
- Set a consistent sleep window, even during a travel-heavy week.
- Limit alcohol close to bedtime. It often worsens airway collapse.
- Try side-sleeping support if your snoring is louder on your back.
Week 2: Add the mouthpiece if needed
If snoring persists and you don’t have red flags, a mouthpiece can be a practical next step. Many designs aim to keep the airway more open by adjusting jaw or tongue position.
When you’re ready to compare products, start here: anti snoring mouthpiece. Look for clear fit guidance, cleaning instructions, and comfort features.
How to judge success
- Snoring volume drops (partner feedback or recording).
- You wake fewer times and feel more restored.
- Less dry mouth and fewer “wired-but-tired” mornings.
Mistakes that waste time (or create risk)
1) Treating snoring like a joke when your body is waving a flag
Relationship humor is common here. Still, repeated gasping or pauses aren’t a punchline. They’re a reason to get evaluated.
2) Trying five gadgets in one weekend
People do this after a burnout week or a long flight. It feels productive, but it hides the real cause. Change one variable at a time.
3) Forcing comfort issues “because it should work”
A mouthpiece that causes significant jaw pain, tooth pain, or bite changes is not a willpower challenge. Stop and reassess. Consider professional guidance.
4) Ignoring infection-control basics
Clean your device as directed. Store it dry. Replace it when worn. Mouth appliances live in a bacteria-friendly environment, so basic hygiene matters.
FAQ
What’s the quickest way to improve sleep quality if snoring is the issue?
Start with position, alcohol timing, and nasal airflow. If those don’t move the needle, a mouthpiece may be the next practical step.
Can an anti snoring mouthpiece help with travel fatigue sleep?
It can, especially if travel pushes you into back-sleeping or worsens mouth breathing. Test it at home first so your trip isn’t the trial run.
What if my partner says the snoring stopped but I still feel exhausted?
Track daytime sleepiness and morning symptoms. Persistent fatigue can point to sleep fragmentation or an underlying sleep disorder that needs evaluation.
CTA: Make the next step simple
If you’re ready to move from guessing to a structured trial, explore mouthpiece options and compare fit styles before you buy.
How do anti-snoring mouthpieces work?
Medical disclaimer: This article is for general education only and is not medical advice. Snoring can be a sign of obstructive sleep apnea or other health issues. If you have choking/gasping, witnessed breathing pauses, severe daytime sleepiness, or heart/blood pressure concerns, talk with a qualified clinician for screening and treatment options.
