- Snoring is having a moment because sleep gadgets, burnout, and “optimization” culture keep pushing sleep into daily conversation.
- Sleep quality matters more than noise. The goal is steadier breathing and fewer wake-ups, not just a quieter room.
- An anti snoring mouthpiece can be a solid middle step between “do nothing” and heavy-duty interventions.
- Not all snoring is equal. Some patterns deserve a medical check, especially when there are breathing pauses or daytime exhaustion.
- Connected-care oral appliances are trending, but the basics still win: fit, comfort, and consistent use.
Why everyone’s talking about snoring again
Sleep is no longer just a wellness checkbox. It’s a productivity tool, a relationship topic, and a travel survival strategy. People compare scores from wearables, swap “sleep hacks” in group chats, and joke about separate bedrooms like it’s a new status symbol.
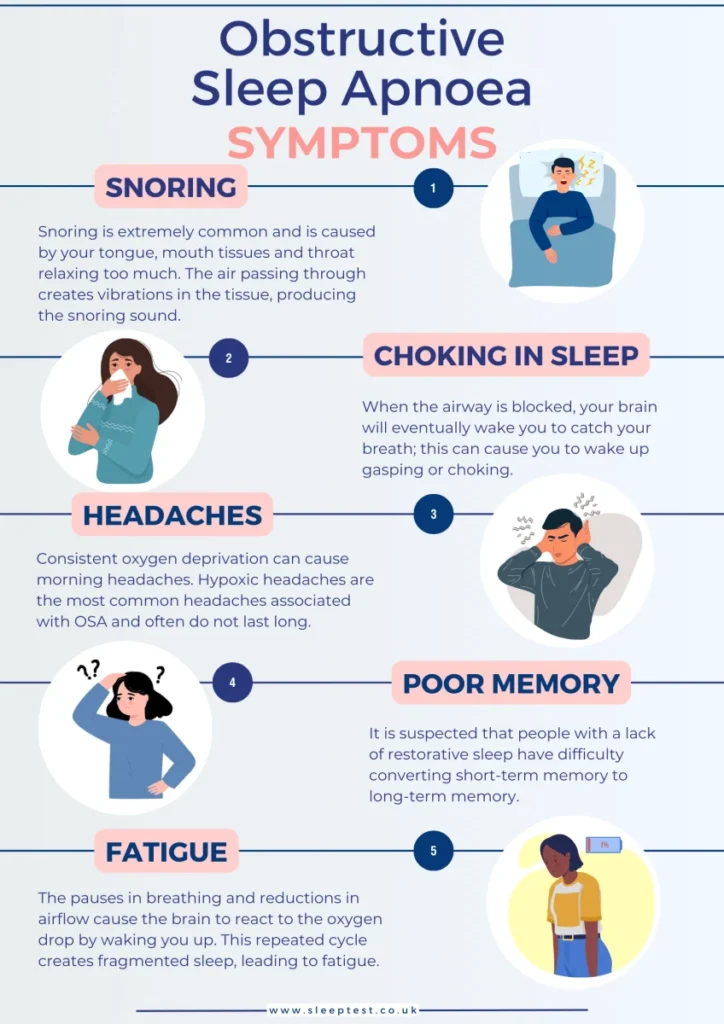
At the same time, major health outlets keep reminding readers that snoring can be more than an annoyance. It can overlap with sleep-disordered breathing concerns, including obstructive sleep apnea. Dental sleep medicine is also getting attention, with professional discussions around new oral-therapy directions and how they may fit into broader care.
If you’re trying to cut through the noise, use the decision guide below.
Decision guide: If…then… what to do next
If your snoring is occasional and tied to a clear trigger…
Then: start with the boring basics for 1–2 weeks. Track what changes your nights: alcohol close to bedtime, congestion, late meals, back-sleeping, or travel fatigue. Many people snore more after red-eye flights, conference weeks, or stressful deadlines.
Why this matters: if the trigger is temporary, you may not need a long-term device. You just need a plan for “high-risk” nights.
If snoring is frequent and your sleep feels thin (even if you get 8 hours)…
Then: consider an anti snoring mouthpiece as a practical next step. For many snorers, the issue is airflow and vibration when tissues relax during sleep. A well-designed oral device can help by supporting jaw or tongue position, which may reduce snoring and improve perceived sleep quality.
Reality check: comfort and fit are everything. The “best” option is the one you can actually wear consistently.
If your partner reports pauses, choking/gasping, or you wake up with headaches…
Then: don’t self-experiment for months. Get evaluated by a clinician. Loud snoring plus breathing interruptions and daytime sleepiness can be a sign of sleep apnea or another sleep-related breathing disorder.
Dental approaches can be part of the conversation, and professional coverage has highlighted January JADA outlines emerging dental therapies for obstructive sleep apnea. Still, screening comes first when red flags show up.
If you’re overwhelmed by sleep gadgets and “viral hacks”…
Then: pick one lane and test it. Wearables, smart pillows, nasal strips, mouth taping, white noise—there’s always a new trend. Some people enjoy experimenting. Others end up more anxious and sleep worse.
Simple rule: choose one change, measure for 10–14 nights, then decide. If you want a device-based option that’s purpose-built for snoring, look at anti snoring mouthpiece rather than stacking five hacks at once.
If relationship tension is the real problem (not just the sound)…
Then: treat sleep like shared infrastructure. Snoring jokes are funny until neither person gets deep sleep. Agree on a plan: track nights, test one intervention, and set a check-in date. That keeps it from turning into nightly negotiations at 1 a.m.
What to look for in an anti snoring mouthpiece (without overcomplicating it)
Fit: A secure fit reduces slipping and improves comfort. Poor fit is the fastest path to a device you stop using.
Comfort for jaw and teeth: Mild adjustment can be normal early on. Ongoing pain, bite changes, or tooth sensitivity are not “powering through” moments.
Breathing compatibility: If nasal congestion is common, address that too. Mouth-breathing patterns and blocked nasal airflow can change how any device feels.
Consistency: A “pretty good” mouthpiece worn nightly often beats a “perfect” one used twice a week.
When to skip DIY and talk to a professional
Move up the ladder if you notice loud nightly snoring, witnessed breathing pauses, waking up gasping, significant daytime sleepiness, or high blood pressure concerns. Those are common reasons clinicians recommend evaluation for sleep apnea.
Also get guidance if you have significant jaw issues, dental work that complicates fit, or persistent discomfort. Dental sleep medicine has expanded, and oral appliances may be part of a broader plan for some people.
FAQ
Is snoring always a sign of sleep apnea?
No. Snoring is common and can be harmless, but loud, frequent snoring plus choking/gasping, witnessed pauses, or heavy daytime sleepiness can be a red flag worth medical evaluation.
What does an anti snoring mouthpiece actually do?
Many mouthpieces gently reposition the lower jaw or stabilize the tongue to keep the airway more open, which may reduce vibration (snoring) and improve airflow during sleep.
Can I use a mouthpiece if I grind my teeth?
Sometimes, but fit and material matter. If you have jaw pain, tooth movement concerns, or significant grinding, a dentist-guided option is safer than guessing.
What if my partner snores, not me?
Treat it like a shared sleep problem. Track patterns (alcohol, congestion, back-sleeping, travel fatigue) and encourage a screening if there are apnea-like symptoms.
Is mouth taping a good idea for snoring?
It’s trending, but it’s not a universal fix and may be unsafe for some people, especially with nasal blockage or suspected sleep-disordered breathing. If you’re curious, discuss it with a clinician.
How fast should a mouthpiece help?
Some people notice changes within a few nights, but comfort and fit can take longer. If symptoms are severe or worsening, don’t wait—get evaluated.
Your next step
If snoring is dragging down your energy, mood, and focus, don’t settle for random hacks. Use a mouthpiece as a structured test: consistent use, simple tracking, and a clear decision point.
How do anti-snoring mouthpieces work?
Medical disclaimer: This article is for general education and does not provide medical advice, diagnosis, or treatment. If you suspect sleep apnea or have concerning symptoms (breathing pauses, chest pain, severe daytime sleepiness), seek care from a qualified clinician.
