On a red-eye flight, “J” promised themself they’d finally fix their sleep. By the time they got home, their feed was full of sleep gadgets, breathing “hacks,” and relationship jokes about snoring on the couch.
That night, the snoring started again. Their partner nudged them, half-laughing, half-exhausted. J reached for a trendy fix they’d seen online—then paused. Viral doesn’t mean safe.
Overview: what’s driving the snoring conversation right now
Snoring is having a moment because people are tired—travel fatigue, workplace burnout, and always-on schedules show up at bedtime. Add the rise of “sleep optimization” content and you get a wave of quick fixes, including mouth-taping and other DIY trends.
Some recent coverage has pushed back on that. If you’ve seen warnings about the mouth-taping trend, the takeaway is simple: restricting breathing during sleep can be risky, especially if you don’t know why you’re snoring.
If you want a more grounded path, an anti snoring mouthpiece is one option many people consider because it aims to improve airflow mechanically rather than blocking it.
For a general reference on the trend discussion, see Scientists warn against viral nighttime mouth-taping trend.
Timing: when to act (and when to stop and screen first)
Use this timing rule: act quickly on comfort and sleep quality, but don’t ignore red flags. If snoring is new, getting worse, or paired with daytime sleepiness, you want screening—not just gadgets.
Fast “do this now” triggers
- Your partner reports loud snoring most nights.
- You wake up unrefreshed, irritable, or foggy.
- Work performance is slipping and you’re blaming “just stress.”
Stop-and-screen triggers (don’t DIY your way through these)
- Choking, gasping, or witnessed pauses in breathing during sleep.
- High blood pressure concerns, morning headaches, or severe daytime sleepiness.
- Snoring plus significant nasal blockage that forces mouth breathing.
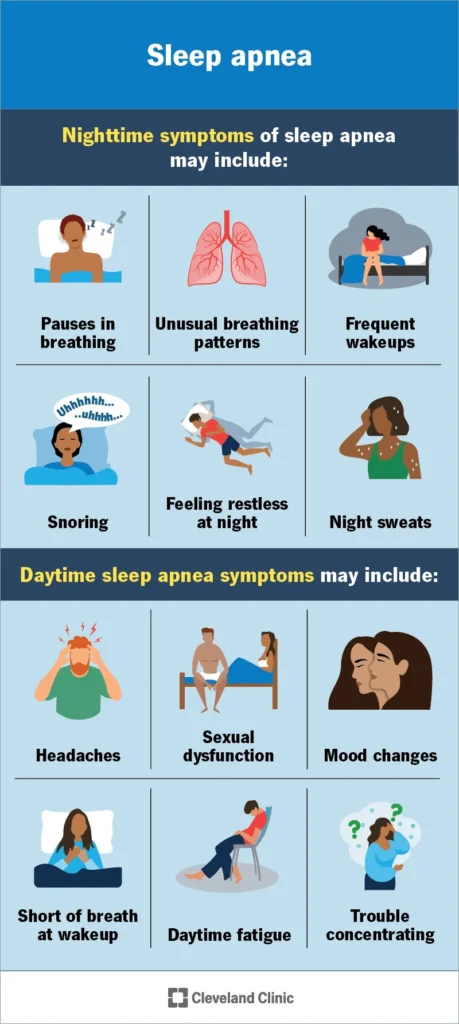
These signs can overlap with obstructive sleep apnea. A clinician can help you sort out causes and options.
Supplies: what you need for a safer, trackable trial
Think “trial with documentation,” not “random experiment.” That reduces risk and helps you decide what’s worth keeping.
- A snoring plan: side-sleeping intent, alcohol timing, and a consistent bedtime window.
- A way to track: a simple notes app, sleep diary, or snore recording app.
- Nasal support if needed: saline rinse or strips (avoid anything that makes breathing feel restricted).
- A mouthpiece option: choose a design that matches your needs and tolerance.
If you’re exploring a combined setup, you can review this anti snoring mouthpiece as one example of a product category people consider.
Step-by-step (ICI): Identify → Choose → Implement
This is the no-drama workflow: identify what’s likely happening, choose a reasonable tool, then implement with guardrails.
1) Identify your snoring pattern
Do a quick 7-night baseline. Note bedtime, wake time, alcohol timing, congestion, and whether you slept on your back. If possible, record snoring volume for a few nights.
Also note symptoms that point beyond “simple snoring,” like morning headaches or heavy daytime sleepiness. If those show up, prioritize screening.
2) Choose the least risky intervention first
Skip anything that restricts breathing. That includes mouth-taping if you’re congested, unsure about apnea risk, or simply uncomfortable with the idea.
Instead, consider options that support airflow:
- Positional changes: side-sleeping often reduces snoring for back-sleepers.
- Nasal comfort: address dryness or congestion so breathing feels easier.
- Anti-snoring mouthpieces: designed to reposition the jaw or tongue to reduce airway collapse.
Consumer chatter about mouthguards often focuses on “does it work?” The better question is: “Is it appropriate for my mouth and my risk level?” If you have TMJ issues, loose dental work, or significant bite concerns, get dental input.
3) Implement like a controlled trial (not a dare)
Use a two-week plan:
- Nights 1–3: short wear time before sleep to get used to the feel. Stop if you get sharp pain.
- Nights 4–7: full-night use if comfortable. Track snoring and morning jaw comfort.
- Week 2: keep conditions steady (same bedtime window, similar caffeine/alcohol timing). Compare to baseline.
Document your choice. Keep the product info, your start date, and any side effects. If you later talk with a dentist or clinician, this history helps.
Mistakes that waste money (or create avoidable risk)
- Using viral hacks as a substitute for screening. If apnea is possible, you want evaluation, not just noise reduction.
- Ignoring pain. Soreness can happen early, but sharp jaw pain, tooth pain, or worsening headaches are stop signs.
- Changing five variables at once. New pillow, new supplements, new mouthpiece, new bedtime—then you can’t tell what helped.
- Assuming snoring is only a “relationship issue.” It’s also a sleep quality issue, and sometimes a health signal.
- Buying without checking fit and return policies. Comfort and adjustability matter more than hype.
FAQ (quick answers)
Can an anti-snoring mouthpiece improve sleep quality?
It can for some people, especially if snoring comes from jaw position and airway narrowing. Better sleep often shows up as fewer awakenings and less partner disturbance.
What if my partner says I still snore with a mouthpiece?
Re-check sleep position, alcohol timing, and congestion. If snoring stays loud or you have red-flag symptoms, get screened for sleep apnea.
Is it normal to feel jaw tightness?
Mild tightness can happen early. Persistent pain, bite changes, or tooth discomfort aren’t something to “push through.”
Next step: get answers without gambling on trends
If you want a simple starting point, focus on two goals: keep breathing easy and make your trial measurable. That’s how you avoid the loop of buying gadget after gadget.
How do anti-snoring mouthpieces work?
Medical disclaimer: This article is for general education only and is not medical advice. Snoring can be a sign of obstructive sleep apnea or other conditions. If you have choking/gasping, witnessed breathing pauses, severe daytime sleepiness, chest pain, or significant jaw/dental issues, talk with a qualified clinician or dentist before trying devices or sleep “hacks.”
