On a Tuesday night, an anonymous couple does the usual wind-down: phone on “sleep mode,” a new wearable charging on the nightstand, and a promise to be “in bed by 10.” Ten minutes later, one person is out cold. The other is staring at the ceiling, listening to a snore that could drown out a hotel hallway ice machine.
By morning, the jokes start (“You were sawing logs again”). But the mood is real. Sleep quality affects patience, focus, and how human you feel at 2 p.m. in a meeting.
What people are talking about right now (and why)
Snoring has moved from “embarrassing quirk” to “sleep health problem to solve.” You see it in the rise of sleep gadgets, travel-recovery content, and workplace burnout conversations. People are trying everything from humidifiers to nasal strips to app-based sleep coaching.
At the same time, more clinics are highlighting noninvasive options for obstructive sleep apnea care, including oral appliances for appropriate patients. And headlines keep connecting untreated sleep-disordered breathing with broader costs like lost productivity and health risks. The takeaway: the snore isn’t just annoying. It can be a signal.
If you want context on why sleep apnea is being framed as a big productivity issue, read this coverage: Sleep Better Marysville Expands Sleep Apnea Treatment Services in Marysville, Ohio with Noninvasive Solutions for Obstructive Sleep Apnea Patients – The Florida Times-Union.
What matters medically (without overcomplicating it)
Snoring happens when airflow gets noisy as it passes through relaxed tissues in your upper airway. That can be as simple as congestion or sleeping on your back. It can also be part of a bigger pattern, like obstructive sleep apnea (OSA).
OSA is not “just snoring.” It involves repeated airway collapse or narrowing that disrupts breathing and sleep. Many articles also discuss links between untreated OSA and long-term health concerns like cardiovascular strain and metabolic issues. You don’t need to panic, but you do want to screen smartly.
Quick self-screen: snoring that deserves extra attention
- Someone witnesses pauses in breathing, choking, or gasping
- You wake with headaches, dry mouth, or feel unrefreshed most days
- Daytime sleepiness (including drowsy driving risk)
- High blood pressure, or you’re treating it but still feel exhausted
- Snoring got noticeably worse with weight changes, alcohol, or sedatives
If several of these fit, a conversation with a clinician or a sleep clinic is the safer next step than buying random gadgets.
What you can try at home (a practical, low-drama plan)
Think of this as a “reduce friction” checklist. You’re aiming to improve airflow and stabilize sleep, not chase perfection.
Step 1: Make your nights less snore-friendly
- Side-sleeping: Back sleeping often worsens snoring. A body pillow can help you stay put.
- Alcohol timing: Alcohol close to bedtime relaxes airway muscles. Earlier is usually better.
- Nasal breathing support: If you’re congested, address the cause (allergies, dryness, irritants). Saline rinses and humidity may help some people.
- Sleep schedule: Travel fatigue and late nights can deepen collapse-prone sleep stages. Consistency helps more than most people expect.
Step 2: Consider an anti snoring mouthpiece (when it’s a reasonable bet)
An anti snoring mouthpiece is often designed to reposition the jaw or stabilize the tongue so the airway stays more open. This can reduce vibration and improve airflow for certain types of snoring.
People like mouthpieces because they’re noninvasive and travel-friendly. They also fit the current “sleep optimization” trend: one small item, potentially big impact. But fit and comfort matter. So does choosing the right type for your anatomy.
If you’re comparing styles and want a starting point, see anti snoring mouthpiece.
Step 3: Set safety guardrails (so you don’t tough it out)
- Go slow: Wear it for short periods at first, then build up.
- Watch your jaw: Mild soreness can happen early. Sharp pain, locking, or persistent pain is a stop sign.
- Respect dental health: Loose teeth, gum disease, or major dental work can change what’s appropriate.
- Track outcomes: Use simple notes: snoring reports from a partner, how you feel at noon, and morning symptoms.
A note on mouth tape (since it’s all over social media)
Mouth taping is trending in sleep circles, but it isn’t a universal “hack.” If your nose is blocked or you might have sleep apnea, taping can be unsafe. If you’re curious, talk with a clinician first and prioritize unobstructed breathing over experiments.
When to seek help (and what “noninvasive” can look like)
If snoring is persistent and your sleep quality is poor, get evaluated. This matters even more if you have the red flags listed earlier. Many communities now have expanded access to sleep services, including noninvasive approaches for the right patients.
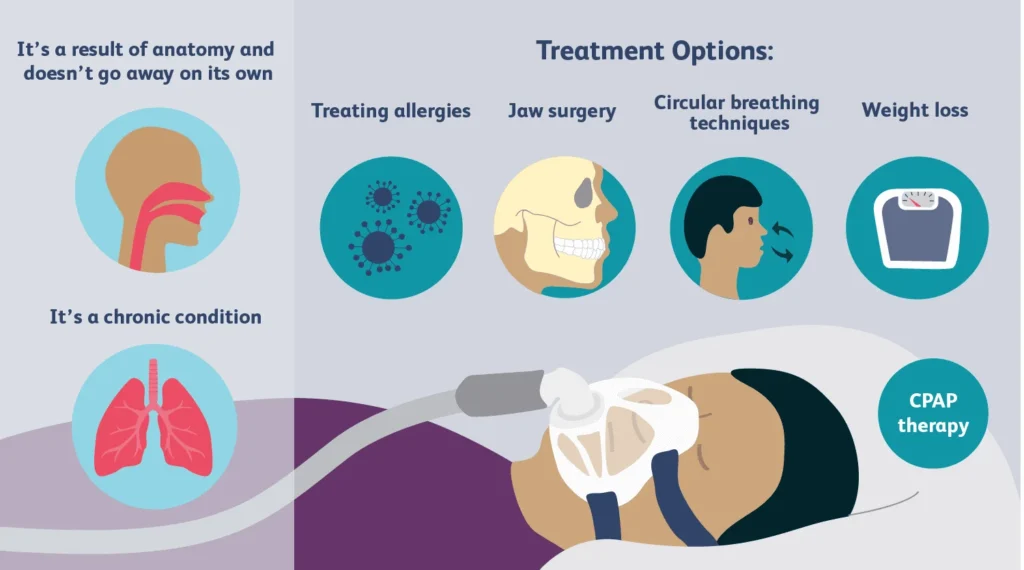
A clinician may recommend a sleep study (at home or in a lab). Depending on results, options may include behavioral changes, CPAP, positional therapy, or a dentist-fitted oral appliance. The goal is effective treatment, not just quieter nights.
FAQ: fast answers for real life
Do anti-snoring mouthpieces work for everyone?
No. They’re a better fit when snoring is related to jaw/tongue position. They’re not a substitute for screening if sleep apnea is suspected.
What’s the difference between snoring and sleep apnea?
Snoring is sound from resistance. Sleep apnea involves repeated breathing interruptions or reductions that fragment sleep and can affect health.
Is mouth taping a safe alternative to a mouthpiece?
Not always. It can be risky if you have nasal obstruction or possible sleep apnea. Ask a clinician before trying it.
How long does it take to get used to an anti-snoring mouthpiece?
Often several nights to a few weeks. Start gradually and stop if pain persists.
When should I talk to a dentist or sleep specialist?
Go sooner if there’s gasping, witnessed pauses, heavy daytime sleepiness, or ongoing high blood pressure. Also go if snoring persists despite basic steps.
Next step: pick one path and document it
If your snoring seems simple and you don’t have warning signs, try a structured at-home plan for two weeks. If you want a compact tool that matches today’s travel-heavy, gadget-filled reality, a mouthpiece may be worth testing.
How do anti-snoring mouthpieces work?
Medical disclaimer: This article is for general education and does not provide medical advice, diagnosis, or treatment. If you suspect sleep apnea or have symptoms like choking/gasping, witnessed breathing pauses, chest pain, severe daytime sleepiness, or uncontrolled blood pressure, seek medical care promptly.
