At 3:07 a.m., someone in a hotel room rolls over, checks the clock, and sighs. The trip was supposed to be a reset. Instead, it’s the familiar combo: travel fatigue, a buzzing brain, and a partner joking (not really joking) about the “chainsaw soundtrack.”
If that feels familiar, you’re not alone. Sleep has become a full-on cultural topic again—gadgets, hacks, and “doctor-approved” routines everywhere. The challenge is turning that noise into a plan that actually improves sleep quality without wasting money on the wrong fix.
What people are talking about right now (and why it’s everywhere)
Recent sleep coverage has clustered around a few themes: waking up in the middle of the night, shifting schedules (hello, daylight savings), and the rise of sleep accessories that promise quick relief. It’s not just about comfort. People are connecting sleep to burnout, mood, focus, and even relationship peace.
There’s also a growing marketplace for anti-snoring devices. That doesn’t automatically mean every product works for every person. It does mean more people are actively looking for practical, at-home options—especially ones that don’t require a whole new bedtime personality.
The “3 a.m. problem” meets the snoring problem
Those middle-of-the-night wake-ups get a lot of attention because they feel so personal and so frustrating. For some sleepers, snoring and subtle breathing disruptions can contribute to fragmented sleep. For others, the wake-up is more about stress, alcohol, temperature, or scrolling in bed.
If you want a general overview of clinician-style sleep hygiene ideas that people keep referencing lately, see this Stop waking up at 3 am — I asked 5 doctors for their best sleep hygiene tips and here’s what they said. Use it as a menu, not a mandate.
What matters medically (without getting lost in jargon)
Snoring usually happens when airflow is partially blocked and soft tissues vibrate. That blockage can come from several places—nose, soft palate, tongue, or jaw position. The “right” fix depends on which factor is doing most of the work.
Here’s the practical takeaway: an anti snoring mouthpiece is most likely to help when jaw or tongue position contributes to airway narrowing during sleep. If your main issue is nasal congestion, the mouthpiece may not be the best first move.
Snoring vs. sleep apnea: don’t guess
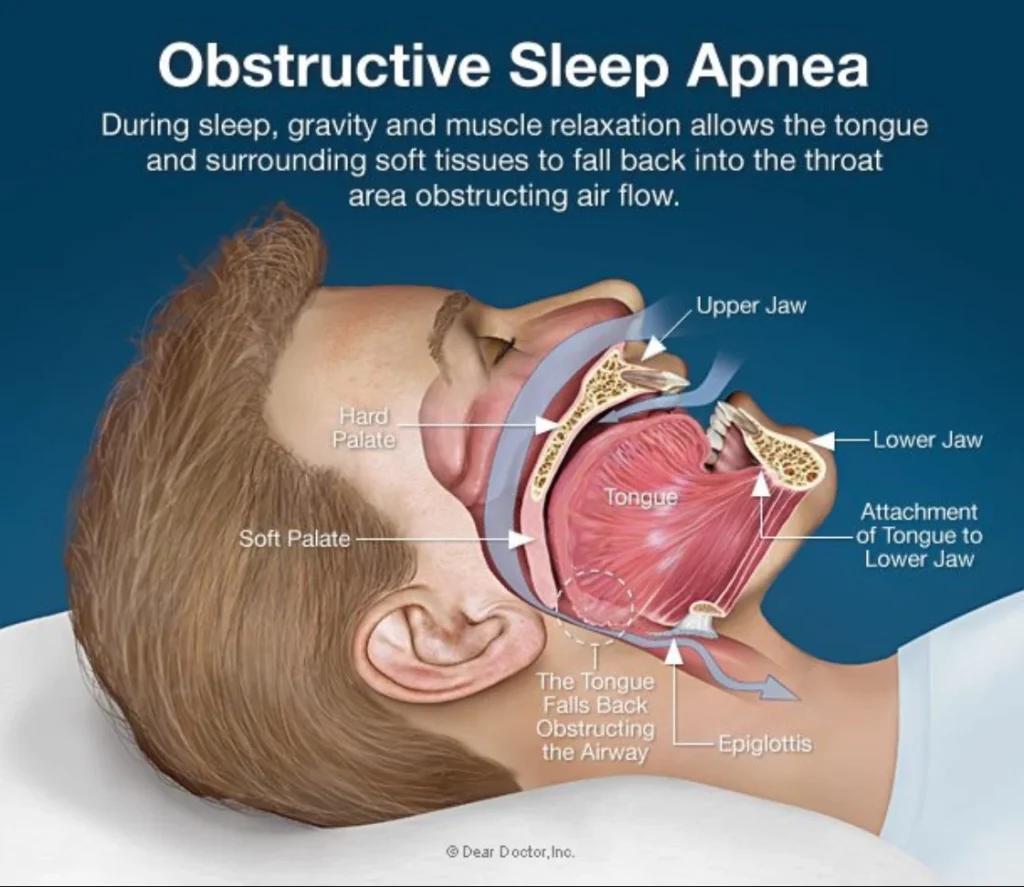
Snoring can be harmless, and it can also be a sign of obstructive sleep apnea. You can’t confirm sleep apnea by sound alone. If you see warning signs—gasping, choking, witnessed pauses in breathing, morning headaches, or strong daytime sleepiness—treat that as a reason to seek medical evaluation.
What you can try at home (budget-first, low-drama)
If you’re trying to improve sleep quality without burning a month on trial-and-error, start with the simplest levers. Make one change at a time so you can tell what actually helped.
Step 1: Run a quick “why am I snoring?” check
Use a short checklist for one week:
- Timing: Is snoring worse after alcohol, heavy meals, or late nights?
- Position: Is it louder on your back than on your side?
- Nasal status: Are you congested or mouth-breathing?
- Daytime feel: Refreshed or wrecked?
This helps you avoid buying a solution for the wrong cause.
Step 2: Clean up the “sleep basics” that amplify snoring
Small changes can reduce snoring intensity and improve sleep continuity:
- Keep alcohol earlier in the evening (or skip it on “test” nights).
- Try side-sleeping support (pillow placement can be enough).
- Set the room cooler and darker than you think you need.
- Protect the last 30–60 minutes from work stress and bright screens.
These aren’t glamorous. They’re also the cheapest.
Step 3: Consider an anti snoring mouthpiece if the pattern fits
If back-sleeping and jaw position seem tied to the noise, a mouthpiece may be worth a focused trial. The goal is simple: support a position that keeps the airway more open so airflow is smoother and less “vibrating.”
When you shop, prioritize clear fit guidance, comfort features, and an approach you can stick with on weeknights. If you want a combined option, you can review this anti snoring mouthpiece.
Step 4: Be cautious with trendy add-ons
Sleep trends come fast. One example is mouth taping, which gets a lot of attention. It may not be appropriate for people with nasal congestion, anxiety around breathing, or possible sleep apnea. If you can’t breathe comfortably through your nose while awake, don’t treat nighttime as the testing ground.
When it’s time to get help (so you don’t “DIY” the wrong problem)
Get medical advice if any of these are true:
- Your partner notices breathing pauses, gasping, or choking sounds.
- You’re excessively sleepy, irritable, or foggy despite enough time in bed.
- You have high blood pressure, heart risks, or persistent morning headaches.
- Snoring is new, rapidly worsening, or paired with weight changes.
A clinician can help rule out sleep apnea and guide you toward options that match your anatomy and health profile.
FAQ: quick answers before you spend another dollar
How do I know if my mouthpiece is fitted well?
A good fit feels secure but not painful. You should be able to sleep without jaw strain, gum soreness, or tooth pain. If discomfort persists, stop using it and reassess.
Can a mouthpiece help relationship sleep drama?
It can reduce the noise that keeps a partner awake. Pair it with practical habits too, like consistent bedtime timing and a cooler room, so both people sleep better.
What if snoring only happens when I’m exhausted or traveling?
That’s common. Travel, dehydration, alcohol, and back-sleeping can all make snoring louder. Pack the simplest tools you’ll actually use, and keep your routine as consistent as possible.
Next step: get a clear, simple explanation
If you’re deciding whether a mouthpiece makes sense, start with the basics and keep it practical. Understanding the “how” prevents impulse buys.
How do anti-snoring mouthpieces work?
Medical disclaimer: This article is for general education and does not provide medical diagnosis or treatment. If you suspect sleep apnea or have significant symptoms (gasping, pauses in breathing, severe daytime sleepiness), seek evaluation from a qualified healthcare professional.
