- Snoring is trending again because sleep gadgets are everywhere, burnout is real, and couples are tired of negotiating pillows.
- Sleep quality is the main issue. The sound is annoying, but the fragmented sleep is what drags your day down.
- An anti snoring mouthpiece can be a practical first step for many people with simple snoring.
- Not all snoring is “just snoring.” Some patterns overlap with sleep apnea symptoms and need medical attention.
- Small home tweaks matter. Position, alcohol timing, nasal airflow, and routine can change your night fast.
What people are talking about right now (and why)
Sleep has become a full-on lifestyle category. Rings score it, apps grade it, and new devices keep popping up in headlines and clinical research. At the same time, work stress and screen-heavy evenings make “good sleep” feel like a moving target.
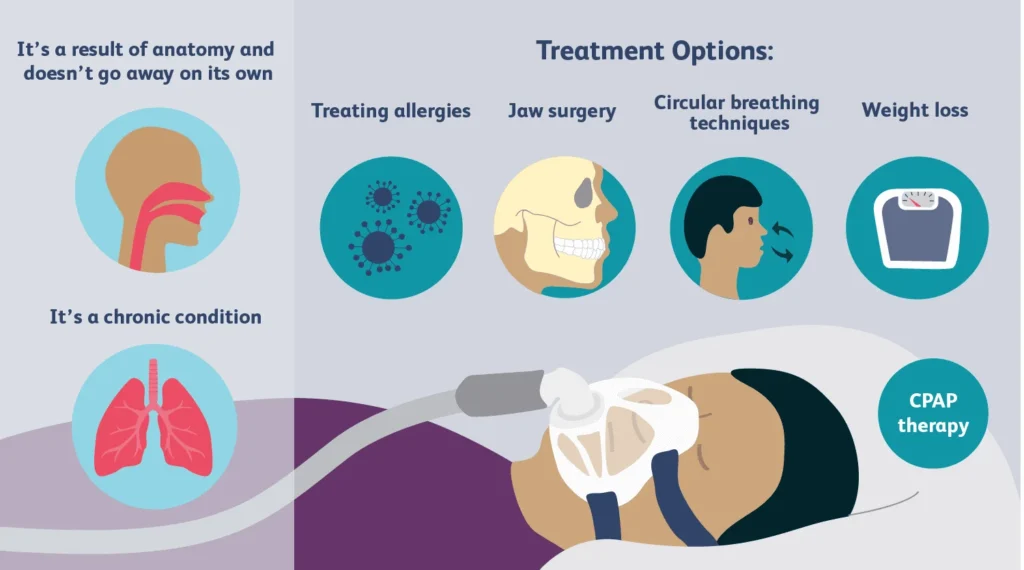
Snoring sits right in the middle of this moment. It’s personal, it’s shareable, and it’s often funny until it isn’t. One partner jokes, the other partner quietly Googles solutions at 2 a.m.
There’s also growing interest in airway-focused dental approaches and new anti-snoring devices being tested. The cultural takeaway: people want options that are simpler than a full medical setup, but more effective than wishful thinking.
If you’re curious about the broader conversation around dental approaches to sleep and breathing, see Creative Smiles Dentistry Advances Airway Dentistry to Address Sleep and Breathing Health in Tucson.
What matters medically (without the drama)
Snoring happens when airflow gets turbulent and soft tissues in the upper airway vibrate. That can show up after a long day, after drinks, during allergy season, or when you sleep on your back.
Here’s the key point: snoring can be harmless, but it can also travel with sleep-disordered breathing. Sleep apnea is a separate medical condition with its own risks and symptoms. If you suspect it, don’t self-manage forever.
Snoring vs. possible sleep apnea: quick pattern check
More “simple snoring” vibes: mostly sound, worse on back, better on side, no choking, you feel okay most days.
More “get checked” vibes: loud snoring plus witnessed pauses, gasping/choking, morning headaches, dry mouth, high sleepiness, or concentration problems.
Medical disclaimer: This article is for general education, not diagnosis or treatment. If you have symptoms of sleep apnea or any serious sleep concerns, talk with a qualified clinician or a sleep specialist.
How to try at home (a clean, realistic plan)
Think in layers. You’re aiming to reduce airway collapse risk and improve airflow, not chase perfect silence.
Layer 1: Remove the common “snore amplifiers”
- Alcohol timing: If you drink, consider stopping earlier in the evening. Many people snore more after late drinks.
- Sleep position: Side-sleeping often reduces snoring for back-snorers.
- Nasal airflow: Congestion and dryness push you toward mouth-breathing. Address allergies and consider simple humidity changes.
- Travel fatigue: After flights or late arrivals, prioritize hydration and a consistent bedtime. A single “rough night” can turn into a snore streak.
Layer 2: Where an anti snoring mouthpiece fits
An anti snoring mouthpiece is popular because it’s tangible and relatively quick to test. Many designs aim to support airflow by gently changing jaw or tongue position during sleep. That can reduce vibration and improve sleep continuity for some people.
Comfort matters as much as the concept. A device that sits in a drawer doesn’t help your sleep score or your relationship.
If you’re comparing options, start here: anti snoring mouthpiece.
Layer 3: Make it stick for 14 nights
- Pick one change at a time (position, nasal routine, or mouthpiece). Stacking everything at once makes it hard to know what worked.
- Track two signals: partner-reported snoring and your daytime energy.
- Watch your jaw comfort: mild adjustment is common, sharp pain is not.
When to stop experimenting and get help
If snoring is paired with choking, gasping, or observed breathing pauses, skip the endless gadget loop. Ask about sleep apnea screening. The same goes for severe daytime sleepiness, drowsy driving risk, or high blood pressure concerns.
Also seek help if you can’t tolerate a mouthpiece, if jaw pain persists, or if you have significant dental issues. A dentist or sleep clinician can help match the approach to your anatomy and symptoms.
FAQ
Do anti-snoring mouthpieces work for everyone?
No. They often help with simple snoring, especially when jaw position and airway space play a role. They may not be enough if you have sleep apnea or significant nasal blockage.
How fast should an anti snoring mouthpiece help?
Many people notice a change within a few nights, but comfort and fit can take a week or two. If snoring is unchanged after consistent use, reassess fit and triggers like alcohol or congestion.
Is loud snoring always a sign of sleep apnea?
Not always, but it can be a clue. If snoring comes with choking/gasping, witnessed breathing pauses, or heavy daytime sleepiness, ask a clinician about sleep apnea screening.
Can travel fatigue make snoring worse?
Yes. Jet lag, alcohol on flights, nasal dryness, and back-sleeping in unfamiliar beds can all increase snoring for a few nights.
What’s the difference between a mouthguard and an anti-snoring mouthpiece?
A sports mouthguard mainly protects teeth. Many anti-snoring mouthpieces are designed to change jaw or tongue position to support airflow during sleep.
Next step (the simplest CTA)
If snoring is hurting your sleep quality, test a plan you can actually follow for two weeks. Start with one or two changes, then add a mouthpiece if it fits your situation.
