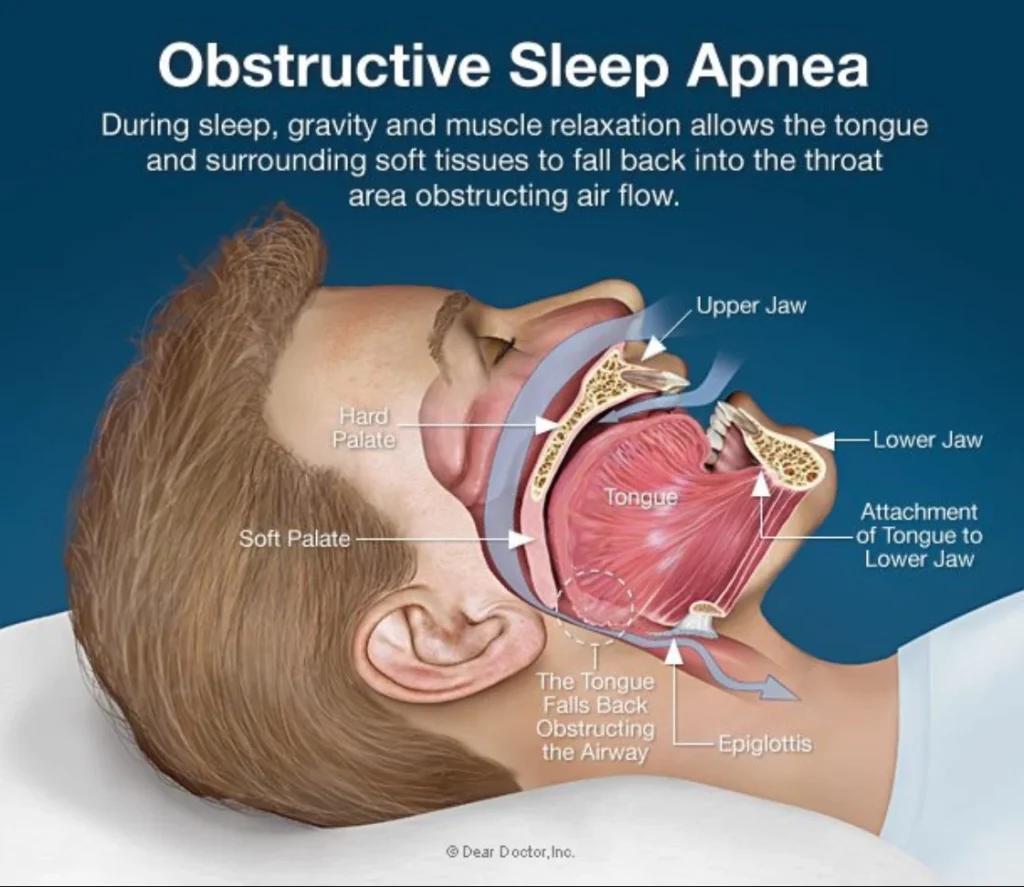
Myth: If you don’t snore, your sleep is fine.
Reality: You can still have disrupted breathing and poor sleep quality even without the “chainsaw soundtrack.” Recent sleep coverage has hammered this point: snoring is a clue, not a guarantee.
Myth: The newest sleep gadget fixes everything.
Reality: Most people do better with one practical change at a time—especially if you’re dealing with travel fatigue, workplace burnout, or a partner who’s started negotiating “quiet hours.”
Big picture: why snoring is suddenly everyone’s topic again
Sleep has become a lifestyle category. There are trackers, smart rings, sunrise lamps, white-noise machines, and apps that grade your night like a performance review. That’s useful—until you start collecting gear instead of solving the problem.
Snoring keeps showing up in conversations because it’s loud, social, and immediate. It affects the snorer and the person next to them. It also ties into the bigger story: sleep quality impacts mood, focus, and how resilient you feel the next day.
One more nuance people are hearing lately: breathing-related sleep issues can exist even when snoring isn’t obvious. If you want a quick read on that idea, see this Yes, You May Have Sleep Apnea Even If You Don’t Snore explainer.
The emotional part: it’s not just noise, it’s friction
Snoring is one of those issues that turns into jokes—until it doesn’t. Couples end up with “pillow walls,” separate rooms on work nights, or travel plans that quietly include a second hotel bed. Nobody wants to be the reason someone else is exhausted.
On the snorer’s side, there’s often embarrassment and defensiveness. On the partner’s side, there’s resentment and sleep debt. The fastest way out is a simple, testable plan with a clear end date.
Practical steps: a no-waste way to test what helps at home
Step 1: Run a 7-night baseline (no new gear)
Don’t change five things at once. For one week, track three basics:
- Snoring impact: Did anyone get woken up? How many times?
- Morning feel: Headache, dry mouth, fogginess, or okay?
- Daytime function: Sleepiness, caffeine dependence, irritability.
Step 2: Clean up the “easy wins” (still cheap)
These aren’t glamorous, but they’re common culprits:
- Alcohol close to bedtime: It can worsen airway collapse for some people.
- Nasal congestion: If you can’t breathe through your nose, you’re more likely to mouth-breathe and snore.
- Sleep position: Back-sleeping often makes snoring louder. Side-sleeping can reduce it for many.
Step 3: If snoring persists, consider an anti snoring mouthpiece
If you’re trying to avoid an expensive gadget spiral, an anti snoring mouthpiece is one of the more direct interventions to test. Many are designed to gently adjust jaw position or help keep the airway more open.
Want to compare styles and features without overthinking it? Start here: anti snoring mouthpiece.
Step 4: Do a 14-night “mouthpiece trial” the right way
Two weeks is long enough to judge comfort and trend lines. Keep it simple:
- Nights 1–3: Expect an adjustment period. Mild drooling or jaw awareness can happen.
- Nights 4–10: Look for fewer wake-ups and less partner disruption.
- Nights 11–14: Decide: keep, modify, or stop.
To avoid placebo math, focus on outcomes you can feel: fewer awakenings, better morning energy, and less “sleep hangover.” If you share a bed, partner feedback matters too.
Safety and testing: when to stop DIY and get checked
Snoring can be benign, but it can also be a sign of a bigger breathing issue during sleep. Don’t push through red flags just to “make the mouthpiece work.”
Get medical advice if you notice any of these
- Choking/gasping episodes during sleep (or someone witnesses breathing pauses)
- Strong daytime sleepiness, especially while driving or sitting still
- Frequent morning headaches
- High blood pressure concerns or heart-risk discussions with your clinician
Dental/jaw guardrails
Stop and reassess if you get sharp jaw pain, tooth pain, gum irritation, or bite changes that don’t fade. Mouthpieces involve your teeth and jaw. A dentist can help you choose a safer path if you have crowns, TMJ issues, or loose teeth.
Medical disclaimer: This article is for general education only and isn’t medical advice. It doesn’t diagnose, treat, or replace care from a qualified clinician. If you suspect sleep apnea or have concerning symptoms, seek professional evaluation.
FAQs: quick answers people keep searching
Is snoring always caused by being “out of shape”?
No. Weight can be one factor, but nasal blockage, jaw anatomy, sleep position, alcohol, and sleep deprivation can also contribute.
Can wearables confirm sleep apnea?
Wearables can hint at poor sleep or breathing irregularities, but they don’t replace clinical testing. Use them as a prompt to get evaluated if symptoms fit.
Should I try multiple anti-snore devices at once?
Usually no. Stacking devices makes it hard to tell what helped and can make sleep more uncomfortable. Test one change at a time.
CTA: one clean next step
If you’re ready to stop guessing and start testing, begin with a mouthpiece-focused plan and track results for two weeks.
