Snoring isn’t just “a funny noise.” It’s a nightly quality-of-life problem.
And lately, it’s getting treated like a tech trend—apps, wearables, nasal gadgets, and sleep scores that judge you before breakfast.
Here’s the real takeaway: you can test practical, low-drama options (including an anti snoring mouthpiece) while still screening for the medical stuff that shouldn’t be ignored.
What people are trying right now (and why)
Sleep has become a lifestyle category. People compare sleep trackers the way they used to compare coffee beans. That means snoring solutions are getting pulled into the same “add to cart” culture.
A few themes keep popping up in the conversation:
- Sleep gadgets everywhere: smart rings, white-noise machines, and “biohacking” routines that promise perfect rest.
- Travel fatigue: red-eyes, hotel pillows, and dry airplane air can make snoring worse for some people.
- Relationship humor: couples joke about “sleep divorces,” but the frustration is real when one person can’t rest.
- Workplace burnout: stress and irregular sleep can amplify snoring and next-day fog.
At the same time, more headlines are nudging people toward evidence-minded questions. For example, researchers have looked at nasal dilators and sleep-disordered breathing in a systematic review. If you want the general source, see this Clinical Effectiveness of Nasal Dilators in Sleep-Disordered Breathing: A Systematic Review and Meta-Analysis.
What matters medically (so you don’t miss the point)
Snoring is airflow plus vibration. Something narrows the airway, tissues flutter, and the sound shows up. That “something” can be temporary or structural.
Common contributors include nasal congestion, sleep position, alcohol close to bedtime, and anatomy. Chronic sinus or nasal issues can also influence sleep quality, and people often notice changes after treatment or surgery for chronic nasal problems.
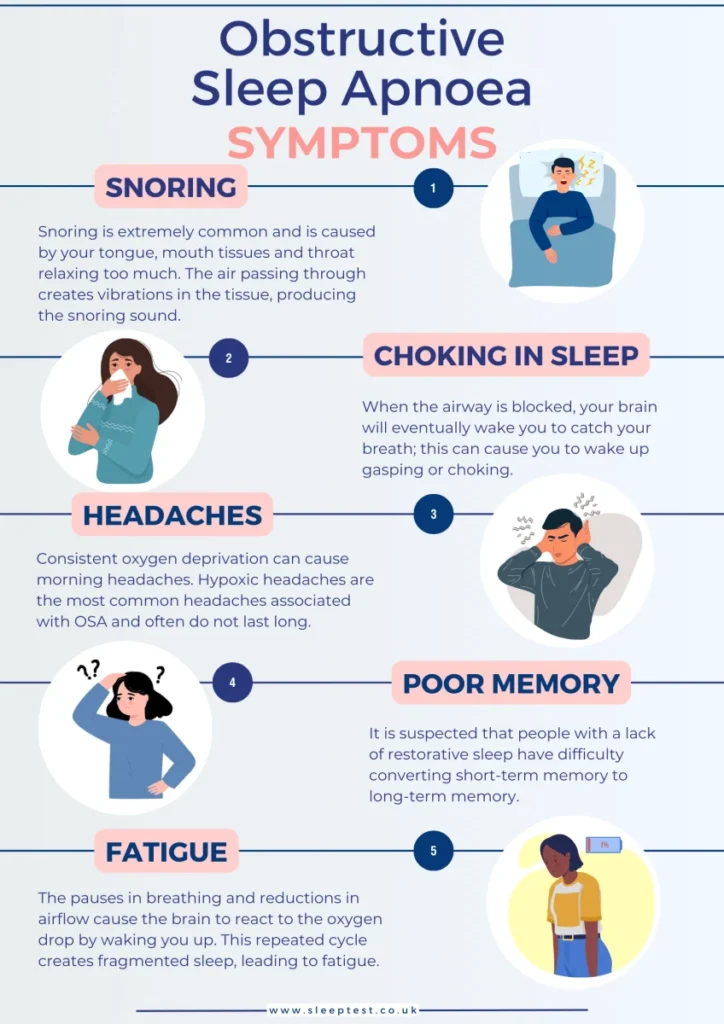
The bigger issue is this: sometimes snoring is paired with obstructive sleep apnea (OSA). OSA is not just “loud snoring.” It involves repeated breathing interruptions during sleep, and it can affect daytime functioning and long-term health. Major medical sources describe hallmark symptoms like loud snoring, gasping, and excessive daytime sleepiness.
So the goal isn’t only “be quieter.” It’s to breathe well, sleep deeply, and wake up functional.
What you can try at home (a low-risk testing plan)
If you’re experimenting, keep it simple. Change one thing at a time. Document what you did and what happened. That protects you from wasting weeks chasing placebo effects.
Step 1: Do a quick baseline check
- Record 2–3 nights of audio (phone on the nightstand works).
- Note morning symptoms: dry mouth, headache, sore throat, jaw tightness, or grogginess.
- Ask the roommate question: “Did you hear pauses or choking?” It’s awkward, but useful.
Step 2: Try the easy airflow wins
Before you buy anything, test basics that often move the needle:
- Side sleeping (a body pillow can help).
- Earlier alcohol cutoff if snoring spikes after drinks.
- Nasal hygiene that’s appropriate for you (avoid anything that irritates your nose).
Step 3: Consider an anti snoring mouthpiece (and set expectations)
An anti snoring mouthpiece typically aims to keep the airway more open by adjusting jaw or tongue position. It’s not a “sleep gadget” in the trendy sense. It’s a mechanical approach.
What a smart trial looks like:
- Start gradual: wear it for short periods before a full night, if the product instructions allow.
- Watch your jaw: mild soreness can happen early on, but sharp pain is a stop sign.
- Track outcomes: snoring intensity, partner reports, and how you feel at 2 p.m., not just at 7 a.m.
If you’re shopping, here’s a relevant starting point for comparison: anti snoring mouthpiece.
When to stop DIY and get checked
Self-testing is fine for simple snoring. It’s not fine when red flags show up.
Consider medical screening if you notice any of the following:
- Witnessed breathing pauses, choking, or gasping during sleep
- Excessive daytime sleepiness or drowsy driving risk
- High blood pressure concerns, morning headaches, or mood changes
- Snoring that persists despite reasonable changes
- Significant nasal blockage, chronic congestion, or post-surgery questions about sleep
Also pause and ask for help if you have TMJ disorder, significant dental work, loose teeth, or ongoing jaw pain. Mouthpieces can be the wrong tool in those situations.
Medical disclaimer: This article is for general education and does not replace medical advice, diagnosis, or treatment. If you think you may have sleep apnea or another sleep disorder, talk with a qualified clinician.
FAQ: quick answers people actually want
Is snoring always a health problem?
No, but it can be. Snoring can be benign, yet it can also signal sleep-disordered breathing. The context and symptoms matter.
What’s more important: snoring volume or how I feel?
Both matter. Loudness affects relationships, but daytime sleepiness, headaches, and concentration issues are bigger health clues.
Can I combine a mouthpiece with a nasal dilator?
Some people do, especially if they suspect both nasal and mouth/throat factors. Start one change first so you can tell what’s helping.
Do mouthpieces cure sleep apnea?
They may help certain cases, but “cure” is not a safe assumption. If apnea is suspected, get evaluated and follow a clinician’s plan.
CTA: choose a plan you can stick to
If your goal is quieter nights and better recovery, skip the hype cycle and run a clean experiment. Pick one intervention, track results, and escalate to screening when red flags appear.
