Myth: Snoring is just a funny relationship problem.
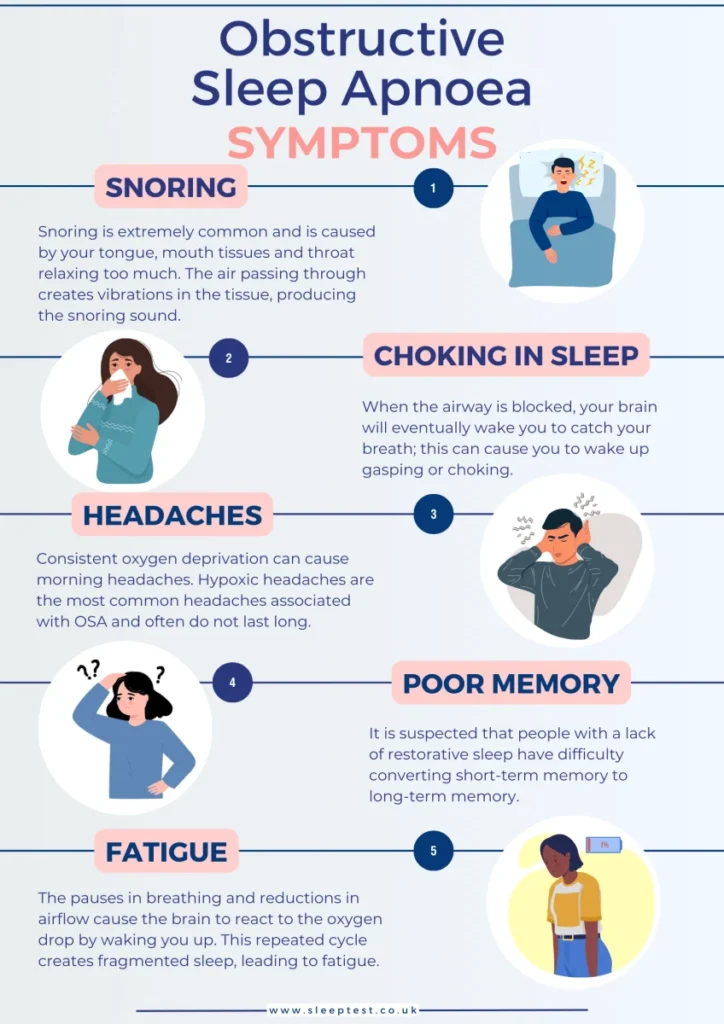
Reality: Snoring can be a sleep-quality problem, a health signal, or both. The right fix depends on what’s causing the noise and whether your breathing is being disrupted.
This guide cuts through the trend cycle—sleep gadgets, “biohacks,” and the latest social-media bedtime routines—and focuses on what you can do safely. If you’re considering an anti snoring mouthpiece, you’ll also get a simple screening checklist to reduce risk and avoid wasting money.
What people are talking about right now (and why it matters)
Sleep is having a moment. You see it in wearable scores, sunrise-alarm clocks, and “doctor-approved” sleep hygiene lists making the rounds. You also feel it after travel fatigue, daylight-saving time shifts, and the kind of workplace burnout that makes 3 a.m. wake-ups feel inevitable.
Snoring sits right in the middle of these trends because it’s public. A partner hears it. A roommate jokes about it. A hotel wall proves it. That’s why mouthpieces, nasal strips, and other quick fixes keep going viral.
Some headlines also point to broader health angles—like questions about vitamin and lifestyle factors, and the ongoing “snoring or sleep apnea?” debate. Keep those references as prompts, not proof. Your body still needs a personalized approach.
What matters medically: snoring vs. sleep apnea (quick screening)
Snoring happens when airflow causes soft tissues in the upper airway to vibrate. It often gets worse with back-sleeping, alcohol close to bedtime, nasal congestion, or weight changes. It can also show up during stressful seasons when sleep timing becomes irregular.
Sleep apnea is different. It involves repeated breathing pauses or shallow breathing that can fragment sleep and strain the body. You can snore without sleep apnea, and you can have sleep apnea without loud snoring.
Red-flag signs you shouldn’t ignore
- Choking, gasping, or witnessed breathing pauses during sleep
- Severe daytime sleepiness, dozing off unintentionally, or drowsy driving risk
- Morning headaches, dry mouth, or unrefreshing sleep most days
- High blood pressure or heart/metabolic concerns (especially with loud snoring)
If these show up, prioritize medical evaluation over DIY experimentation. Mouthpieces can still be part of a plan, but you want the right diagnosis first.
How to try at home (low-risk steps before you buy anything)
You don’t need a drawer full of gadgets to start. Use a two-week test window and change one variable at a time. That helps you document what actually moves the needle.
Step 1: Track the problem like a grown-up (simple, not obsessive)
- Pick 2–3 markers: wake-ups, morning grogginess, partner-reported snoring, or a basic snore recording.
- Note triggers: late alcohol, heavy dinner, congestion, back-sleeping, travel days, or high-stress workweeks.
Step 2: Reduce the “easy” airflow blockers
- Nasal breathing support: manage congestion (saline rinse, humidity, allergy control if relevant).
- Sleep position: side-sleeping often reduces snoring for back-sleepers.
- Timing: keep alcohol and sedating meds away from bedtime when possible (ask your clinician before changing prescriptions).
Step 3: Use proven sleep-hygiene basics to lower 3 a.m. wake-ups
Many people chase snoring fixes when the bigger issue is fragmented sleep. If you’re dealing with early-morning wake-ups, a practical routine can help you fall asleep faster and stay asleep longer. For a mainstream roundup of clinician-style guidance, see 6 Natural Remedies for Sleep Apnea That Improve Your Breathing.
Where an anti snoring mouthpiece fits (and how to choose safely)
An anti-snoring mouthpiece typically works by repositioning the lower jaw and/or stabilizing the tongue so the airway stays more open. This can reduce tissue vibration and cut down snoring for the right person.
Who tends to benefit most
- Snoring that’s worse on the back
- Snoring linked to jaw/tongue collapse (not just nasal congestion)
- People who want a non-machine option and can tolerate a dental device
Safety and screening checklist (reduce the “oops” factor)
- Dental health: avoid use if you have loose teeth, untreated gum disease, or significant dental pain.
- Jaw history: TMJ disorder, jaw clicking with pain, or limited opening needs caution.
- Fit and materials: follow cleaning instructions and replace as recommended to reduce irritation and hygiene issues.
- Document changes: track comfort, morning bite changes, and daytime sleepiness. Stop if symptoms worsen.
What to look for in a product description
- Clear sizing/fit guidance and comfort features
- Return policy (important if you can’t adapt)
- Easy cleaning and durable construction
If you’re comparing options, start here: anti snoring mouthpiece.
When to seek help (so you don’t miss the bigger problem)
If snoring is paired with major daytime fatigue, witnessed breathing pauses, or high-risk health factors, don’t self-treat indefinitely. A clinician can screen for sleep apnea and guide next steps.
Also get help if a mouthpiece causes ongoing jaw pain, tooth discomfort, gum irritation, or changes in how your teeth fit together in the morning that don’t resolve quickly. Comfort is not a “tough it out” category when your bite is involved.
FAQ: fast answers before you decide
Is loud snoring always a health problem?
Not always, but it can signal airway narrowing or sleep disruption. Treat it as worth checking, especially if you feel tired or your partner notices breathing irregularities.
Do vitamins fix snoring?
Vitamin status can matter for overall health, but snoring usually has mechanical and lifestyle drivers. If you suspect a deficiency, confirm with a clinician rather than guessing.
What if my snoring is worse after travel or daylight-saving time?
Sleep timing shifts, alcohol, and congestion can all stack the deck. Reset your schedule, prioritize nasal breathing, and revisit your baseline after a week.
CTA: pick a plan you can stick with
If your screening looks low-risk and your goal is fewer snores and better sleep continuity, a mouthpiece may be a practical next step—especially if position changes and basic sleep hygiene aren’t enough.
How do anti-snoring mouthpieces work?
Medical disclaimer: This article is for general education and isn’t medical advice. It doesn’t diagnose, treat, or replace care from a qualified clinician. If you suspect sleep apnea or have significant daytime sleepiness, chest pain, or breathing pauses during sleep, seek medical evaluation.
