You don’t need a sleep lab to know something is off. If snoring is the nightly soundtrack, your “8 hours” can still feel like a loss.
Right now, the smartest approach is simple: follow the trends, but make choices that protect sleep health and screen for risk.
What people are talking about right now (and why it matters)
Sleep is having a moment. New wearables score your “readiness,” travel schedules wreck routines, and burnout makes even a full night feel thin. Meanwhile, couples trade jokes about separate bedrooms like it’s a relationship hack.
Alongside the gadgets, there’s growing interest in attention and sleep challenges. Recent coverage has highlighted how people with ADHD often struggle with consistent sleep routines and winding down. That overlap matters because fragmented sleep can amplify focus issues the next day.
There’s also buzz around quick fixes, including mouth taping. Articles have questioned whether it helps and who should avoid it. The takeaway: viral hacks aren’t automatically safe, and snoring needs a more grounded plan.
If you want a broader look at routine-building ideas, see How to Improve Sleep When You Have ADHD.
What matters medically: snoring isn’t always “just annoying”
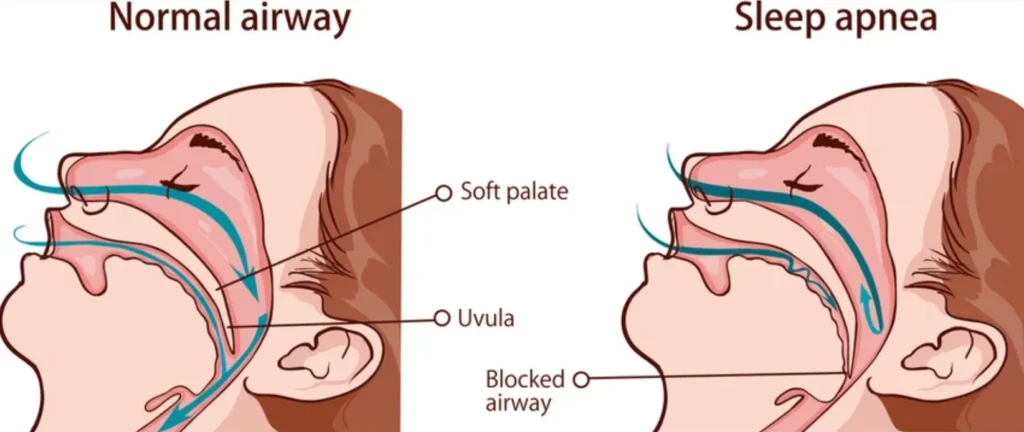
Snoring happens when airflow gets noisy as it moves through a narrowed airway. That narrowing can come from sleep position, alcohol, congestion, weight changes, or anatomy.
Sometimes, though, snoring is a sign of obstructive sleep apnea (OSA). OSA involves repeated breathing disruptions during sleep. Major medical organizations note that sleep apnea is linked with serious health risks, including heart concerns, so it’s worth taking seriously.
Fast self-screen: check for red flags
- Loud snoring most nights
- Witnessed pauses in breathing
- Waking up choking, gasping, or with a racing heart
- Morning headaches or dry mouth
- Daytime sleepiness, dozing off easily, or near-miss driving fatigue
- High blood pressure or heart disease history
If several apply, treat snoring as a health question, not just a noise problem.
What you can try at home (low-drama, high-signal)
You want changes you can actually stick to. Aim for a two-week experiment and write down what you did. This helps you avoid “I think it helped?” guessing later.
Step 1: reduce the common triggers
- Side-sleeping: Back sleeping often worsens snoring.
- Alcohol timing: Avoid alcohol close to bedtime if snoring is an issue.
- Nasal support: Address congestion with simple, non-medicated options when appropriate (like saline rinse). Follow product labels.
- Wind-down consistency: A repeatable routine beats a perfect routine.
Step 2: consider an anti snoring mouthpiece (with a safety checklist)
An anti snoring mouthpiece is designed to improve airflow by changing jaw or tongue position during sleep. For many people, the appeal is obvious: it’s non-surgical, portable, and doesn’t require power. It also fits the “travel fatigue” reality when hotel pillows and time zones already stack the odds against you.
Before you buy or use one, document your baseline:
- How many nights per week you snore (estimate)
- How often your partner nudges you or leaves the room
- Morning symptoms (headache, sore throat, dry mouth)
- Daytime energy (1–10)
Step 3: choose a product path you can follow
If you’re exploring a combined approach, you can review this anti snoring mouthpiece. Keep expectations realistic: comfort, fit, and consistency usually determine whether people keep using it long enough to see benefit.
Important: be cautious with mouth taping
Mouth taping is trending, but it’s not a universal snoring solution. If you have nasal blockage, reflux, panic symptoms, or possible sleep apnea, taping can be a bad idea. When in doubt, skip it and choose a safer, reversible option.
When to stop DIY and get checked
Get medical guidance if you suspect sleep apnea or if your symptoms escalate. You should also seek help if you have jaw pain, tooth pain, or bite changes with any mouthpiece. Those are signals to pause and reassess.
Consider asking about a sleep evaluation if snoring comes with daytime sleepiness, breathing pauses, or high blood pressure. A clinician can help you decide whether a home sleep test or another assessment makes sense.
FAQ
Can an anti snoring mouthpiece help if I’m just a “light snorer”?
It can, especially if snoring is worse on your back or after alcohol. Results vary, and you should screen for sleep apnea red flags first.
Is snoring always sleep apnea?
No. Snoring can come from nasal congestion, sleep position, alcohol, or anatomy. But loud, frequent snoring with breathing pauses can signal sleep apnea.
What’s the difference between a mouthpiece and mouth taping?
A mouthpiece changes jaw or tongue position to keep the airway more open. Mouth taping aims to encourage nasal breathing, but it isn’t a snoring treatment for everyone and can be risky for some people.
How long does it take to know if a mouthpiece works?
Many people can tell within several nights to a few weeks. Track snoring volume, awakenings, and daytime sleepiness to judge real change.
Who should not use an anti-snoring mouthpiece without medical advice?
People with suspected sleep apnea, significant jaw pain/TMJ issues, loose teeth, major dental work in progress, or anyone who wakes up choking or gasping should talk to a clinician first.
CTA: make your next step easy
If snoring is starting to affect your sleep quality, relationship, or workday focus, don’t wait for a “perfect” week to act. Pick one change, track it, and build from there.
How do anti-snoring mouthpieces work?
Medical disclaimer: This article is for general education only and is not medical advice. Snoring can be a sign of obstructive sleep apnea or other conditions. If you have choking/gasping, breathing pauses, chest pain, severe daytime sleepiness, or heart concerns, seek care from a qualified clinician.
