Snoring is having a moment. Not the fun kind.
Between sleep trackers, “morning routine” trends, and travel fatigue, more people are noticing how one noisy sleeper can tank the whole household.
Thesis: Better sleep quality starts with spotting what kind of snoring you have—then choosing the simplest tool that matches the risk.
What people are talking about right now (and why it matters)
Sleep advice is everywhere. Experts keep circling back to the basics: consistent schedules, less late-night scrolling, and treating sleep like a health pillar, not a luxury.
At the same time, gadgets are booming. Rings, watches, white-noise machines, smart pillows, and “mouth tape” debates show up in feeds daily. Add workplace burnout and constant travel, and plenty of people are running on fumes.
Then there’s relationship humor. The “one of us snores” jokes land because they’re true. Snoring doesn’t just disrupt the snorer. It can chip away at the other person’s deep sleep too.
If you want a quick scan of the kind of mainstream guidance people share and search for, see this roundup-style reference: How to improve sleep habits in children: Doctor shares tips, says sleep is as important as nutrition and immunization for kids.
The medically important part: snoring vs sleep apnea
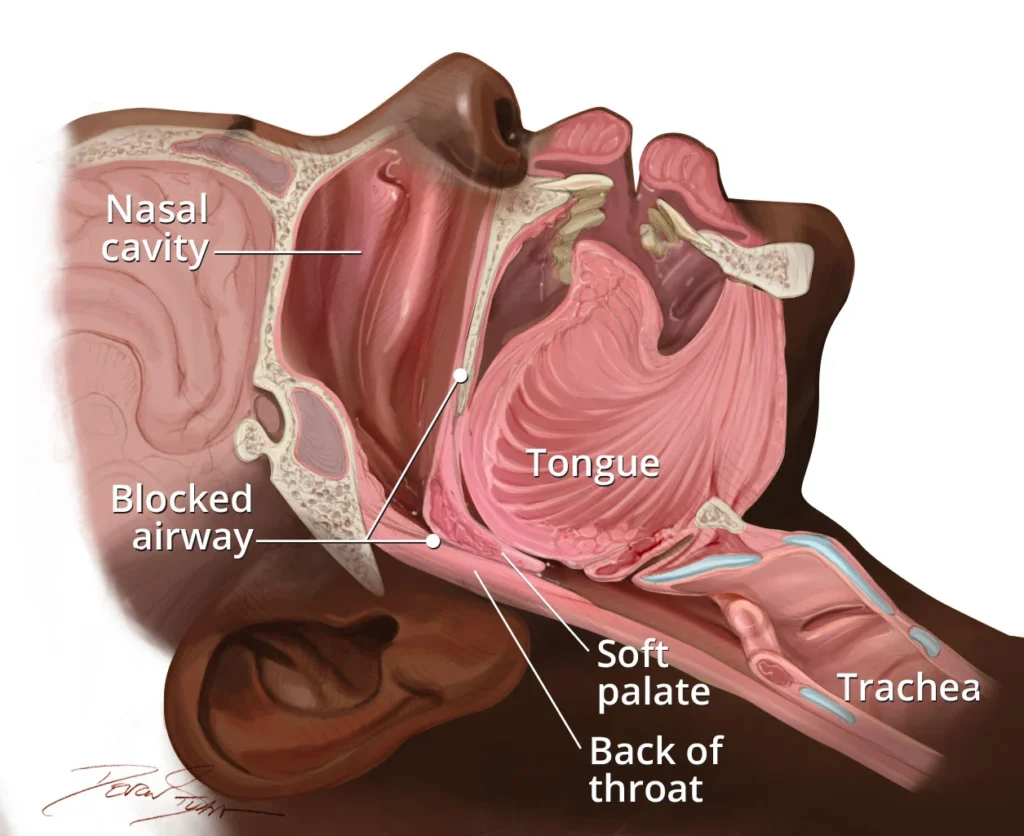
Snoring happens when airflow is partially blocked and tissues vibrate. That can be “simple snoring,” or it can be a sign of something more serious.
Sleep apnea is different. It involves repeated breathing interruptions during sleep. General medical sources describe common clues like loud snoring, gasping or choking, witnessed pauses in breathing, and significant daytime sleepiness.
Why the distinction changes your next step
If it’s simple snoring, a targeted tool (like an oral device) plus habit tweaks may be enough. If it’s possible sleep apnea, you’ll want a proper evaluation because untreated apnea can affect overall health and daytime safety.
Medical note in plain language: this article can’t diagnose you. If you suspect apnea, don’t “DIY” your way past the red flags.
Try-this-at-home plan (low effort, high signal)
Think of this as a two-week experiment. You’re looking for a clearer pattern, not perfection.
1) Do a quick “snore audit”
Pick 3 data points and track them for 10–14 nights:
- Position: back vs side sleeping.
- Timing: alcohol, heavy meals, or intense workouts close to bedtime.
- Symptoms: dry mouth, morning headaches, daytime sleepiness, or waking up startled.
If you travel for work, note that too. Hotel air, jet lag, and new pillows can make snoring spike.
2) Protect sleep quality first
When burnout is high, people chase fancy fixes and forget the boring stuff that works. Aim for:
- Consistent wake time most days.
- A wind-down buffer (even 20 minutes).
- Less alcohol close to bedtime, if you notice it worsens snoring.
- Addressing nasal congestion (saline rinses or other options your pharmacist/clinician says are safe for you).
3) Consider an anti snoring mouthpiece if the pattern fits
An anti snoring mouthpiece is designed to improve airflow by changing jaw or tongue positioning during sleep. People often look at these when snoring is frequent, position-dependent, and disruptive, but without obvious apnea warning signs.
If you want a streamlined option that pairs oral support with a stabilizing strap, you can review an anti snoring mouthpiece.
Comfort matters. A device you can’t tolerate won’t help your sleep quality, even if it’s “technically effective.”
When to stop experimenting and get checked
Skip the guesswork and talk with a clinician if any of these show up:
- Witnessed breathing pauses, choking, or gasping during sleep.
- Excessive daytime sleepiness, dozing while driving, or brain fog that’s affecting work.
- High blood pressure or heart concerns, especially with loud nightly snoring.
- Snoring plus morning headaches or waking up unrefreshed most days.
For children, regular snoring deserves a pediatric evaluation. Recent health conversations increasingly emphasize that sleep supports growth, learning, and immune function, so it’s worth addressing early.
FAQ: quick answers for real-life sleepers
Do anti-snoring mouthpieces work for everyone?
No. They often help with simple snoring, especially when snoring is worse on your back. They may not be enough if you have sleep apnea or significant nasal blockage.
How fast should an anti snoring mouthpiece help?
Many people notice a difference within a few nights. Give it about 1–2 weeks to judge comfort, fit, and whether snoring and sleep quality improve.
Is loud snoring always sleep apnea?
Not always. But loud snoring plus choking/gasping, witnessed pauses, or daytime sleepiness raises concern for sleep apnea and is worth medical evaluation.
Can a mouthpiece cause jaw pain?
It can, especially early on or if the fit is off. Mild soreness may settle as you adapt, but persistent pain, tooth movement, or bite changes should be checked by a dentist or clinician.
What else helps snoring besides a mouthpiece?
Side sleeping, reducing alcohol close to bedtime, treating nasal congestion, and keeping a consistent sleep schedule can all help. Weight changes may also affect snoring for some people.
Should kids use anti-snoring mouthpieces?
Only with guidance from a pediatric clinician or pediatric dentist. Kids who snore regularly should be evaluated because causes and treatments differ from adults.
CTA: make tonight quieter (without overthinking it)
If snoring is dragging down your sleep quality, keep it simple: pick one habit change and one tool to test for two weeks. Track the results. Adjust based on what you learn.
How do anti-snoring mouthpieces work?
Medical disclaimer: This content is for general education and is not medical advice. It does not diagnose, treat, or replace care from a qualified clinician. If you suspect sleep apnea or have severe symptoms, seek professional evaluation.
